Social Competence in Children with Neurofibromatosis Type 1: Relationships with Psychopathology and Cognitive Ability
Amelia K Lewis, Melanie A Porter, Tracey A Williams, Kathryn N North and Jonathan M Payne
DOI10.4172/2472-1786.100020
1Department of Psychology, Macquarie University, Sydney, New South Wales, Australia
2Centre for Atypical Neurodevelopment, Macquarie University, Sydney, New South Wales, Australia
3ARC Centre of Excellence in Cognition and Its Disorders, Macquarie University, Sydney, New South Wales, Australia
4Kids Rehab, The Children’s Hospital at Westmead, Sydney, New South Wales, Australia
5Murdoch Children’s Research Institute, The Royal Children’s Hospital, Melbourne, Victoria, Australia
6Department of Paediatrics, Faculty of Medicine, Dentistry and Health Sciences, University of Melbourne, Melbourne, Victoria, Australia
- *Corresponding Author:
- Melanie Porter
Department of Psychology, Macquarie University NSW 2109, Australia
Tel: +61 2 9850 6768
E-mail: melanie.porter@mq.edu.au
Received Date: January 29, 2016 Accepted Date: March 14, 2016 Published Date: March 21, 2016
Citation: Lewis AK, Porter MA, Williams TA, et al. Social Competence in Children with Neurofibromatosis Type 1: Relationships with Psychopathology and Cognitive Ability. J Child Dev Disord. 2016, 2:12.doi: 10.4172/2472-1786.100020
Abstract
Background: Neurofibromatosis type 1 (NF1) is a neurodevelopmental disorder associated with elevated risk of specific cognitive impairments and a high prevalence of psychological comorbidities. Children with NF1 have also been reported to display significant difficulties with peer relationships, although the exact nature of their social competence difficulties remains unclear. This study aimed to explore the nature of the day to day social competence difficulties observed in children with NF1 and to investigate how these difficulties might relate to cognitive dysfunction and symptoms of psychopathology.
Methods and Findings: This study investigated parent ratings of day to day social competence in 23 children with neurofibromatosis type 1 (NF1) compared to 23 chronological age-matched typically developing controls using a brief, standardised questionnaire - the Social Competence with Peers Questionnaire. The relationships between social competence, psychopathology (parent ratings of Attention Deficit Hyperactivity Disorder or Autism Spectrum Disorder symptomatology), and cognitive ability (Full Scale IQ and parent ratings of functional executive behaviour) in children with NF1 were also explored using correlational analyses. Results indicated that children with NF1 displayed significantly poorer day to day social competence than controls. These social competence deficits were not related to Attention Deficit Hyperactivity Disorder symptomatology, Full Scale IQ or functional executive behaviour. However, difficulties with social competence were significantly related to Autism Spectrum Disorder symptomatology and socially anxious/avoidant behaviours in our NF1 cohort.
Conclusions: These results indicate that children with NF1 are at significant risk of day to day social competence difficulties, especially those who display high levels of autistic symptomatology and socially anxious behaviour. Our findings suggest a need to incorporate screening for social competence problems and comorbid psychopathology into the more general clinical management of children with NF1.
Keywords
Social competence; Neurofibromatosis type 1; Psychopathology; Cognition
Introduction
Neurofibromatosis type 1 (NF1) is an autosomal dominant genetic disorder with an estimated prevalence of approximately 1 in 3,000. The condition is caused by a mutation of the NF1 gene on the long arm of chromosome 17 [1, 2] and is associated with distinctive physical characteristics, neurofibromas (benign tumours); skinfold freckling; café-au-lait macules (pigmented birthmarks) and Lisch nodules (melanocytic hamartomas affecting the iris) [3]. There is considerable variability in the clinical presentation of children with NF1 [4], however common complications of the condition include specific cognitive impairments [5, 6] and a high prevalence of psychological comorbidities [7, 8]. Poor social skills and difficulties with interpersonal relationships have also been reported in NF1 [9, 10], although the latter is particularly under-researched. As such, the aim of the current study was to investigate, in greater detail, the nature of day to day social competence difficulties in children with NF1. A second and related aim was to investigate how levels of social competence in children with NF1 might relate to cognitive dysfunction and/or symptoms of psychopathology.
Specific cognitive impairments
Cognitive impairment is widespread in NF1, affecting approximately 80% of children with the condition [5]. Deficits in attention, visuospatial skills, language, and executive function (including planning, organisation, inhibition, and self-monitoring) are most common [5, 11-13]. In contrast, intellectual functioning typically falls broadly within the normal range, although a distinct and reliable downward shift in overall intelligence levels compared with both the general population and unaffected sibling controls has been consistently reported [5, 14, 15]. Academic difficulties are also common, with between 50 and 70% of children with NF1 demonstrating impairments in literacy or numeracy skills [16, 17] and approximately 20% estimated to meet criteria for a learning disability [17].
Psychological comorbidities
Recent studies have documented a wide range of psychological disorders associated with NF1 [7, 18]. Reports indicate that Attention Deficit Hyperactivity Disorder (ADHD) occurs in 30% to 50% of individuals with NF1 [5, 19, 20]. This is high compared to the rate of approximately 5% in the general population [21]. Children with NF1 also display a significantly higher prevalence of autism spectrum disorder (ASD) symptomatology compared to the general population, with three recent studies reporting that between 11% and 29% of children with NF1 are rated within the severe range on the Social Responsiveness Scale [22] (a screening measure of ASD symptomatology); a range which is strongly associated with a clinical diagnosis of ASD [7, 23, 24]. Importantly, however, NF1 is associated with impairments in several domains that overlap with ASD (including delayed social, executive, and language skills), and so the true prevalence of ASD in NF1 may be lower than these reports would indicate [25]. Nevertheless, a recent population-based epidemiologic study of children and adolescents in with NF1 using diagnostic assessment tools estimated a population ASD prevalence of 24.9% [26], well above the estimated general population prevalence of 1.5% [27].
In addition to ADHD and ASD, there is some evidence to suggest a predisposition towards anxiety disorders in children with NF1 [18]. The prevalence of anxiety disorders in the adult NF1 population has been estimated at between 1% and 6% [28], which is generally in keeping with the rates observed in the general population [29]. Nevertheless, Pasini et al. [18] showed that children and adolescents with NF1 display significantly higher levels of anxiety symptomatology on a self-report measure compared to healthy controls, although these children did not differ significantly from controls on any disorder-specific subscales, including: physical symptoms; harm avoidance; social anxiety and separation panic. The authors noted a moderate correlation between social anxiety symptoms and disease severity, such that participants with more severe physical manifestations of NF1 reported significantly higher levels of social anxiety [18]. Notably, however, significant anxiety (and particularly social anxiety) has been documented in ADHD [30, 31] and ASD [32, 33], making it difficult to tease apart these psychological comorbidities in children with NF1.
Social skills in NF1
Research addressing social functioning in NF1 is in its infancy and has tended to focus primarily on social information processing (especially emotion recognition skills), emotional problems, and social behaviour [34, 35]. For example, Huijbregts and De Sonneville [6] found that children with NF1 display significantly higher levels of emotional, conduct and peer-related problems compared to typically developing controls. Their NF1 cohort also performed significantly worse than controls on social information processing tasks that required them to identify and match facial expressions of emotion. In keeping with these findings, specific emotion recognition deficits have been documented in children with NF1, with Huijbregts et al. [34] showing that children and adolescents with NF1 demonstrate significant difficulty recognising and matching facial expressions of fear and anger. The same emotion recognition deficits have also been documented in the adult NF1 population, with additional deficits evident in identifying whether conversational exchanges were sincere or sarcastic [36].
In general, informant reports of social and emotional functioning in children with NF1 indicate a high incidence of social and behavioural problems [6, 9, 37, 38]. Furthermore, several studies have documented discrepancies between self-report ratings of social skills and informant (parent and teacher) ratings, suggesting that children with NF1 may perhaps lack awareness of their own social and behavioural difficulties [9, 37]. Similar patterns have been documented in adults with NF1, who have been reported to display less prosocial behaviour than the normal population, as well as reduced awareness of their deficits in social skills [35]. Taken together, these findings suggest deficits in aspects of social awareness, social perception and social cognition in this population.
Social competence in NF1
Anecdotally, children with NF1 demonstrate considerable social difficulties on a day to day level, with reports from children with NF1 and their parents suggesting that they are often teased and rejected by their peers and have difficulty forming and maintaining friendships [39]. Nevertheless, only two studies to date have directly examined social competence in children in NF1. Barton and North [9] investigated social skills and social outcomes in children with NF1 using parent and teacher ratings on the Social Skills Rating System (SSRS) [40] and the Child Behaviour Checklist (CBCL) [41]. Children with NF1 were rated by both parents and teachers as having significantly poorer social competence compared with their unaffected siblings, despite there being no significant difference between the groups in terms of their general social skills, including: cooperativeness; assertiveness; responsibility and self-control. The presence of ADHD was found to significantly increase the risk of social competence problems in children with NF1, with those with a comorbid ADHD diagnosis1 performing significantly worse on measures of social competence; they also displayed significantly greater difficulty with social skills and social problems. In keeping with these findings, Noll and colleagues [10] found that children and adolescents with NF1 had significantly fewer reciprocal friendships and were rated as less well liked by their peers compared to their typically developing classmates, despite being rated by teachers and peers as being more prosocial. Parents also rated children with NF1 as having significantly greater difficulties with social competence on the CBCL. The authors noted that social difficulties in their sample appeared to be the most severe for those children with comorbid learning difficulties and / or ADHD; however, this was not formally addressed statistically [10].
There is some evidence to suggest that general cognitive ability may be related to social and behavioural functioning in NF1, although the exact nature of the relationship between social competence and cognitive ability in this population remains unclear. Huijbregts and De Sonneville [6] reported that deficits in general cognitive ability (a composite score comprising measures of processing speed, social information processing, and cognitive control) contributed significantly to emotional problems and reduced social responsiveness in children and adolescents with NF1. Nevertheless, the impact of specific cognitive impairments on day to day social competence (for example, the role of executive dysfunction) requires further investigation. Notably, NF1 is associated with significant functional executive difficulties, with particular deficits evident in sustaining working memory, self-monitoring, and planning and organisation [12]. Executive function and social competence have been shown to be significantly related in the typically developing population [42,43], and in other developmental disorders, including ASD [44], but no published study to date has directly investigated the relationship between executive function and social competence in NF1.
Previous research on social competence in children with NF1 has relied heavily on the Social Problems and Social Competence indices of the CBCL [9, 10, 38]. While this is a valid, reliable, standardised and commercially available measure, only four items across both of these indices directly address the quantity and quality of children’s friendships with their same-age peers2, with the remainder of the items relating to behaviour and personality characteristics (e.g. “dependent”, “clumsy”), as well as family relationships and participation in teams and organisations. As such, the precise nature of the social competence problems reported in children and adolescents with NF1 remains unclear and warrants further investigation. Furthermore, no published studies to date have directly explored whether interpersonal relationships in NF1 are associated with cognitive and/or psychological impairment. It is extremely important to identify the nature of social competence problems in children with NF1 and potential cognitive and psychological risk factors, as this information will assist clinicians working with these children in selecting appropriate screening measures and providing targeted intervention recommendations.
Aims of the current study
In light of the above, the primary aim of the present study was to gain a more comprehensive understanding of day to day social competence in children with NF1 using the parent form of the Social Competence with Peers Questionnaire (SCPQ-P) [1], a nine item questionnaire with excellent psychometric properties which was specifically designed to explore interpersonal relationships, perceived popularity, and involvement in social activities in school-aged children. In keeping with previous findings [9, 10], it was hypothesised that, overall, children with NF1 would demonstrate poorer social competence compared with their typically developing peers (Hypothesis 1). However, given the variability observed in the clinical phenotype of children with NF1 [4, 45], significant variability in their social competence was also anticipated (Hypothesis 2).
The second aim of this study was to examine the relationships between social competence and ADHD and ASD symptomatology in children with NF1. Although previous studies have indicated poorer social skills and social competence in children with NF1 and comorbid ADHD [9, 10], the potential influence of autistic traits on social outcomes in NF1 has received little empirical attention. As up to one quarter of children with NF1 demonstrate significantly elevated symptoms of both ADHD and ASD [7], it is important to determine to what extent ADHD and ASD symptomatology are contributing to social competence problems in NF1. Conversely, it is also important to determine whether or not social competence difficulties exist in NF1 in the absence of comorbid psychopathology. It was hypothesised that reduced social competence would be identified even in children with NF1 and no psychological diagnosis (Hypothesis 3). It was also hypothesised that higher levels of both ADHD and ASD symptomatology would be related to poorer social competence in children with NF1 (Hypothesis 4).
The final aim of the present study was to investigate the relationship between social competence and cognitive functioning in children with NF1, particularly general intellectual functioning (FSIQ) and executive function. It was hypothesised that social competence would not be related to overall levels of intellectual functioning in children with NF1 (Hypothesis 5). In keeping with observations from typically developing children [42, 43], it was hypothesised that social competence would be related to day to day executive function in children with NF1, such that children with more executive difficulties would display lower social competence (Hypothesis 6).
Methods
Participants
NF1 participants in this study were recruited through the Neurogenetics Clinic at The Children’s Hospital at Westmead (CHW), Sydney, Australia. This clinic has a wide referral base and caters for over 1300 individuals with NF1, with all socioeconomic groups represented. Questionnaires were provided to the parents of 30 children with NF1 who were participating in additional research studies at CHW from January 2011 to February 2014. These children met the following inclusion criteria: (a) confirmed diagnosis of NF1 based on criteria specified by the National Institutes of Health Consensus Conference [46]; (b) absence of diagnosed intracranial pathology (e.g. epilepsy, traumatic brain injury, or brain tumour); (c) an IQ ≥ 70; (d) no current or previous diagnosis of anxiety disorder, mood disorder, or psychotic disorder; and (e) competency in the English language. No NF1 participants had to be excluded based on these criteria. Of the 30 sets of questionnaires provided, seven were not returned, leaving a final sample of 23 children with NF1 (15 females, 8 males) aged between 6.67 and 13.83 years (M = 10.04, SD = 2.12). The ‘no response’ group (6 females, 1 male) had a mean age of 10.82 years (SD = 1.55) and a mean FSIQ of 90.43 (SD = 12.93), and did not differ significantly from the participants included in the present study on any demographic variables (all, p > 0.10). A review of clinical records revealed that five NF1 participants had a diagnosis of ADHD. No NF1 participant had a diagnosis of ASD. For NF1 participants, Full Scale IQ (FSIQ) was established using the Wechsler Intelligence Scale for Children - Fourth Edition (WISC-IV) [47].
Twenty-three typically developing (TD) controls (9 females, 14 males) were recruited through Neuronauts: a kids’ science club at Macquarie University, Sydney, Australia. TD participants were aged between 6.67 and 13.42 years (M = 9.92, SD = 1.97). TD control children were excluded from the study if they had a history of developmental delay, IQ < 70, sensory impairments, diagnosed neurological or psychiatric disorder, or English as a second language. No TD controls had to be excluded based on these criteria. As a screening measure, FSIQ was estimated for TD control participants using the Wechsler Abbreviated Scale of Intelligence (WASI) [48].
NF1 and TD control groups were matched for chronological age (within 6 months of age) at the individual level and handedness at the group level. Table 1 displays the demographic characteristics of each group. As shown in Table 1, a chi-square test revealed no significant difference in sex distribution between the groups, although a non-significant trend was observed. Independent samples t-test revealed the two groups were well matched in terms of age. Consistent with literature showing downward shifts in FSIQ in NF1 [5, 14, 15], the two groups differed significantly in terms of their FSIQ scores, albeit on different measurement instruments. On average, the NF1 group fell within the low average IQ range and the TD control group fell within the average IQ range. Overall, the clinical sample was considered to be adequately representative of the wider NF1 population and the TD group were considered to be typically developing.3
| NF1 groupMean (SD)Range | TD groupMean (SD)Range | t score | p value | |
|---|---|---|---|---|
| Males : Females | 8 : 15 | 14 : 9 | 3.136* | 0.077 |
| Chronological Age | 10.04 (2.12) 6.67 – 13.83 |
9.92 (1.97) 6.67 – 13.42 |
0.210 | 0.835 |
| FSIQ | 87.48 (10.33)a 71.00 – 109.00 |
107.61 (12.40)b 79.00 – 134.00 |
-5.981 | <0.001 |
Note: Chronological age is in years. FSIQ scores from both the WISC-IV and WASI are standardised against a normative mean of 100.00 and a standard deviation of 15.00.
* Chi-square statistic
aFSIQ measured using WISC-IV
bFSIQ measured using WASI
Table 1: Demographic characteristics for each group.
Materials
Both groups
Social competence with peers questionnaire - parent form (SCPQ-P)
Social competence was assessed using the SCPQ-P [1], a nine item questionnaire addressing the quality and quantity of children’s friendships, perceived popularity, the nature of their relationships with children of the same age, and their involvement in social activities (e.g. being invited to parties and seeing friends at weekends). Items are rated on a three-point Likert scale from 0 (not true) to 2 (mostly true), with higher scores indicating greater social competence. The psychometric properties of this scale are very respectable, with a reported Guttman split-half reliability coefficient of 0.87 and coefficient alpha of 0.81 [1]. The SCPQ-P was developed to elicit parental assessment of social competence difficulties in school-aged children, with the goal of providing details for targeted intervention for children with social problems. As such, it is well-suited to the investigation of social competence in a clinical population.
There are normative data for the SCPQ-P for children aged between 8 and 17 years [1]. In this sample, the mean parent rating was 14.82 / 18 (SD = 3.12), and there was no effect of age or gender. However, as the sample in the present study included 6 and 7 year old, it was considered most appropriate to compare results against a sample individually matched for chronological age.
NF1 Group
Conners 3 - parent long form (Conners 3-PL)
The Conners 3-PL [49] was administered to the NF1 group. The Conners 3-PL is a standardised, commercially available measure used to assist in the evaluation, diagnosis and treatment response of children with ADHD. It provides standardised scores of ADHD symptoms, as well as comorbid disorders including Oppositional Defiant Disorder and Conduct Disorder. The scale comprises 105 items, each rated on a four-point Likert scale from 0 (not at all true) to 3 (very much true), with higher scores indicating greater difficulty. These items contribute to six separate content scales: Inattention, Hyperactivity / Impulsivity, Learning Problems, Executive Functioning, Defiance / Aggression, and Peer Relations. Raw scores are converted into T-scores based on age and gender norms. T-scores between 60 and 64 are considered “elevated” and are associated with more concerns than is normal, while T-scores ≥ 65 on each scale are “very elevated” and indicate significant areas of concern.
Social responsiveness scale (SRS) parent form
The parent form of the SRS [22] was administered to the NF1 group. The SRS is an instrument designed to identify social difficulties and symptoms of autism spectrum disorders in children and adolescents aged between 4 and 18 years. The SRS comprises 65 items that form five separate treatment subscales: Social Awareness, Social Cognition, Social Communication, Social Motivation (including socially anxious and avoidant behaviours), and Autistic Mannerisms. Items are rated on a four-point Likert scale from 1 (never true) to 4 (almost always true) and raw scores are converted into T-scores based on gender norms, with higher scores indicating greater social difficulties. Scores obtained across the treatment subscales are summed to provide a SRS total score. Total SRS T-scores between 60 and 75 (mild to moderate range) indicate clinically significant levels of autistic traits and are typical for children with less severe ASD [22]. Total SRS T-scores of 76 or more (severe range) indicate a severe interference in everyday social interactions and are strongly associated with the presence of ASD. At the treatment subscale level, T-scores ≥ 60 are considered clinically significant and suggest that a particular area may require treatment or intervention [22]. The SRS has respectable psychometric properties and has previously been used to investigate autism spectrum symptomatology in populations with NF1 [7, 23, 24].
Behavior rating inventory of executive function (BRIEF) - parent version
Parents / guardians of the NF1 group completed the BRIEF [50]. The BRIEF comprises 86 items aimed at assessing day to day executive abilities. These items contribute to eight separate subscales: Inhibit Shift, Emotional Control, Initiate, Working Memory, Plan / Organize, Organization of Materials, and Monitor. Scores on the Inhibition, Shift, and Emotional Control subscales are summed to provide a Behavioral Regulation Index, and scores on the remaining subscales are summed to provide a Metacognition Index. A global composite score (Global Executive Composite) is also generated, incorporating all eight subscales. Raw scores on all indices are converted into T-scores based on age norms, with higher T-scores indicating more problematic behaviours. T-scores ≥ 65 are considered clinically significant. The BRIEF has high internal consistency (0.80 to 0.98) and high testretest reliability [51].
Wechsler intelligence scale for children - fourth edition (WISCIV)
The WISC-IV [47] is one of the most widely used measures of intelligence for children aged between 6 and 16 years. The WISC-IV is made up of ten core subtests which contribute to four composite indices (Verbal Comprehension, Perceptual Reasoning, Working Memory, and Processing Speed), as well as a global FSIQ score. The test takes between 60 and 80 minutes to administer. There are published WISC-IV Australian norms, with scores standardized against a mean of 100 and a standard deviation of 15.
Results
Data were analysed using Predictive Analytics SoftWare (PASW) Version 18 for Windows. Initial investigations revealed that data were not normally distributed and that there was unequal variance between groups, so non-parametric analyses were used. Mean raw scores on the SCPQ-P and standardised T-scores on the SRS, Conners 3-PL, and BRIEF subscales were compared between groups using the Mann-Whitney U test. Relationships between social competence, Conners 3-PL ratings, SRS ratings, BRIEF ratings, and FSIQ in the NF1 group were examined using Spearman’s rho correlations. Correlations were based on SCPQ-P raw scores and standardised (age-adjusted) scores for all other measures. This was considered to be appropriate, as a previous normative study revealed that there was no effect of age on SCPQ-P ratings in a typically developing sample aged between 8 and 17 years [1]. Furthermore, statistical investigations revealed that there was no relationship between age and SCPQ-P raw scores in the present NF1 sample (ρ = -0.161, p = 0.463).
Due to the relatively small sample size in the present study, a p value of .05 was used for all analyses to indicate statistical significance in order to reduce the likelihood of Type II error [52].
Do children with NF1 display lower and more variable social competencies than their TD peers?
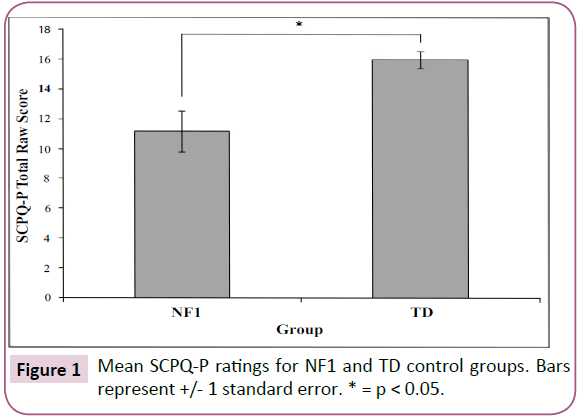
Figure 1 shows the mean social competence ratings for NF1 and TD control groups. On the SCPQ-P, the NF1 group displayed significantly lower overall social competence ratings compared to TD controls (Z = -2.59, p = 0.010)4. Moreover, Levene’s test for equality of variances revealed significantly greater variability in total social competence ratings for the NF1 children compared with the TD control group (F = 20.73, p < 0.001).
Item-level analyses revealed that NF1 children displayed significantly lower ratings on the following items compared to controls: ‘has at least one close friend’ (Z = -3.29, p = .001), ‘has stable friendships with other kids his/her age’ (Z = -2.77, p = 0.006), ‘finds it easy to make friends’ (Z = -2.31, p = 0.021), ‘has good relationships with classmates’ (Z = -2.34, p = 0.020), ‘is popular amongst others his/her age’ (Z = -3.16, p = 0.002), and ‘sees a friend or friends socially at weekends’ (Z = -2.62, p = 0.009). Ratings were similar between NF1 and TD groups on the following items: ‘other kids invite him/her to their homes’ (Z = -1.88, p = .060), ‘other kids invite him/her to social events or activities’ (Z = -1.89, p = 0.059), and ‘gets invited to parties’ (Z = -1.69, p = .090).
To address the possibility of bias due to gender effects on SCPQ-P ratings, correlations between these variables were examined for the NF1 and TD control groups. There was no significant effect of gender on SCPQ-P ratings (both, p ≥ 0.236).
Do those children with NF1 who do not have co-morbid ADHD or ASD demonstrate social competence difficulties?
To determine whether NF1 participants with no comorbid ADHD or ASD diagnosis demonstrate social competence difficulties, the previous analyses were repeated after exclusion of the five NF1 participants with a comorbid psychological diagnosis (ADHD). Even after exclusion of those participants with psychological comorbidities, the NF1 group displayed significantly lower overall social competence ratings compared to TD controls (Z = -2.01, p = 0.045). Again, Levene’s test for equality of variances revealed significantly greater variability in total social competence ratings for the NF1 children compared with the TD control group (F = 9.65, p = 0.004).
General performance on psychological and cognitive questionnaire measures
Conners 3-PL ratings in the NF1 group
Table 2 shows the mean Conners 3-PL ratings for the NF1 group and the percentage of the sample falling within the “very elevated” or clinical range (mean T-scores ≥ 65) on each subscale. On average, the NF1 group displayed very elevated ratings on the domains of Inattention and Learning Problems relative to the normative population. However, parent ratings of Hyperactivity/ Impulsivity, Executive Functioning, Defiance/Aggression, and Peer Relations were within normal limits (mean T-scores < 65).
| Mean (SD) Range |
% in Very Elevated Range | |
|---|---|---|
| Inattention | 66.61* (14.30) 45.00 – 90.00 |
43.5% |
| Hyperactivity/Impulsivity | 62.52 (16.49) 42.00 – 90.00 |
39.1% |
| Learning Problems | 69.91* (12.85) 49.00 – 90.00 |
56.5% |
| Executive Functioning | 61.09 (12.50) 38.00 – 86.00 |
39.1% |
| Defiance/Aggression | 54.70(13.73) 41.00 – 90.00 |
21.7% |
| Peer Relations | 62.70 (16.41) 43.00 – 90.00 |
39.1% |
Note: T-scores have a mean of 50 and a standard deviation of 10. Scores ≥ 65 on the Conners 3–PL represents areas of clinical significance.
* T-score ≥ 65
Table 2: Mean T-scores on the Conners 3–PL for the NF1 group.
Social responsiveness scale ratings in the NF1 group
Table 3 shows the average SRS profiles for the NF1 group. Notably, 17.4% of the NF1 group fell within the severe range (total T-score > 75), a range which is typically associated with a clinical diagnosis of ASD. The most commonly reported difficulties in the NF1 group were related to Social Motivation (socially anxious and avoidant behaviours), which were clinically elevated in 43.5% of the NF1 sample. This was followed by Autistic Mannerisms (e.g. unusually narrow range of interests, repetitive behaviours), which were clinically elevated in 39.1% of the NF1 group.
| Mean (SD) | % in Clinical Range | ||
|---|---|---|---|
| Range | Mild to Moderate (60 ≤ T < 76) |
Severe (T > 75) |
|
| Social Awareness | 55.52 (13.72) 38.00 – 91.00 |
26.1% | 4.3% |
| Social Cognition | 57.61 (15.87) 36.00 – 92.00 |
21.7% | 17.4% |
| Social Communication | 58.65 (13.99) 42.00 – 88.00 |
21.7% | 17.4% |
| Social Motivation | 57.52 (12.58) 40.00 – 89.00 |
34.8% | 8.7% |
| Autistic Mannerisms | 63.39* (18.24) 40.00 – 105.00 |
13.0% | 26.1% |
| SRS Total Score | 60.09 (15.49) 41.00 – 93.00 |
26.1% | 17.4% |
Note: T-scores have a mean of 50 and a standard deviation of 10. T-scores ≥ 60 are considered clinically elevated.
* T-score ≥ 60
Table 3: Mean T-scores on the social responsiveness scale (SRS) for the NF1 group.
BRIEF ratings in the NF1 group
Table 4 shows the average BRIEF ratings for the NF1 group. On average, the NF1 group fell within normal limits on all BRIEF indices (all mean T-scores < 65). The most commonly reported domain of difficulty was Working Memory (occurring in almost 40% of the cohort), followed by Initiate, Shift and Plan / Organize.
| Mean (SD) Range |
% in Clinically Significant Range | |
|---|---|---|
| Inhibit | 52.83 (12.58) 38.00 – 87.00 |
17.4% |
| Shift | 55.74 (14.79) 39.00 – 88.00 |
30.4% |
| Emotional Control | 52.52 (14.15) 36.00 – 80.00 |
17.4% |
| Behavior Regulation Index | 53.91 (13.80) 36.00 – 86.00 |
21.7% |
| Initiate | 58.39 (12.26) 40.00 – 79.00 |
34.8% |
| Working Memory | 60.26 (11.09) 36.00 – 81.00 |
39.1% |
| Plan/Organize | 58.61 (11.40) 41.00 – 80.00 |
30.4% |
| Organization of Materials | 54.87 (11.04) 37.00 – 71.00 |
26.1% |
| Monitor | 57.74 (10.22) 40.00 – 75.00 |
21.7% |
| Metacognition Index | 59.43 (11.31) 39.00 – 81.00 |
34.8% |
| Global Executive Composite | 57.78 (12.35) 38.00 – 80.00 |
30.4% |
Note: T-scores have a mean of 50 and a standard deviation of 10. T-scores ≥65 on the BRIEF represent areas of significant difficulty.
Table 4: Mean t-scores on the behavior rating inventory of executive function in the NF1 group
Correlations
Spearman’s rho correlations were conducted to explore the relationships between social competence and Conners 3-PL ratings, SRS ratings, BRIEF ratings, and FSIQ. Correlations are displayed in Table 5.
| Spearman’s correlation (ρ) | p value | |
|---|---|---|
| Conners 3–PL Content Scores | ||
| Inattention | 0.020 | 0.930 |
| Hyperactivity/Impulsivity | 0.186 | 0.395 |
| Learning Problems | -0.156 | 0.478 |
| Executive Functioning | -0.218 | 0.317 |
| Defiance/Aggression | 0.087 | 0.693 |
| Peer Relations | -0.802 | <0.001** |
| Social Responsiveness Scale Scores | ||
| Social Awareness | -0.069 | 0.753 |
| Social Cognition | -0.283 | 0.191 |
| Social Communication | -0.415 | 0.049* |
| Social Motivation | -0.591 | 0.003** |
| Autistic Mannerisms | -0.422 | 0.045* |
| SRS Total Score | -0.426 | 0.042* |
| Behavior Rating Inventory of Executive Function | ||
| Behavior Regulation Index | -0.016 | 0.944 |
| Metacognition Index | -0.165 | 0.452 |
| Global Executive Composite | -0.112 | 0.612 |
| FSIQ | 0.036 | 0.870 |
* Correlation significant at the p < 0.05 level
** Correlation significant at the p < 0.01 level
Table 5: Correlations between social competence (SCPQ–P) and FSIQ, Conners 3–PL ratings, SRS ratings, and BRIEF ratings for NF1 participants
Does social competence relate to psychopathology (ADHD and ASD symptomatology) in NF1?
The relationships between social competence and ADHD symptomatology (Conners 3-PL ratings of Inattention and Hyperactivity/ Impulsivity) and ASD symptomatology (SRS ratings) in the NF1 group were investigated. No significant associations were identified between ADHD symptoms (Inattention, Hyperactivity/Impulsivity) and SCPQ-P ratings for NF1 participants (both, p > 0.395). SCPQ-P ratings were significantly and negatively correlated with total levels of autistic symptomatology (SRS Total Score; p = 0.048) and also with the SRS Social Communication (p = 0.049), Social Motivation (p = 0.003) and Autistic Mannerisms (p = 0.045) subscales.
Does social competence relate to cognition in NF1?
The relationships between social competence, FSIQ, and day to day executive function (BRIEF and Conners 3-PL Executive Functioning scale ratings) in the NF1 group were also investigated. SCPQ-P ratings were not significantly correlated with FSIQ (p = 0.870). Furthermore, SCPQ-P ratings were not significantly correlated with parent ratings of executive function on the BRIEF subscales and indices (all, p > 0.05) or the Conners 3-PL Executive Functioning content scale (all, p > 0.05).
Discussion
The aims of this study were threefold: (1) to investigate the nature of social competence in children with NF1, (2) to explore relationships between social competence and psychopathology in NF1, and (3) to examine the relationships between social competence, cognition and behaviour in NF1. In relation to the first aim, in line with our hypothesis (Hypothesis 1), the social competence of children with NF1 differed significantly from that of typically developing children. Children with NF1 were rated by their parents as having significantly poorer overall social competence, replicating findings from previous studies using less comprehensive measures [9,10,38]. However, the present study extended existing findings by providing additional information as to the specific nature of these social competence deficits. At the group level, children with NF1 had significantly greater difficulty forming and maintaining friendships, had poorer overall relationships with their classmates, were less popular than their same-age peers, and were less likely to see friends outside of school compared with TD controls. Notably, scores on the SCPQ-P were strongly correlated with scores on the Conners 3-PL Peer Relations scale, supporting its validity as a measure of social competence for children with NF1. As predicted (Hypothesis 2), there was significantly greater individual variability in social competence ratings among children with NF1 when compared with the TD control group, with some NF1 children falling in the normal range, and others demonstrating significant impairments in day to day social competence. This indicates that certain children with NF1 are more vulnerable to social difficulties than others.
In relation to the second aim, 47.8% of NF1 children were rated as having significantly elevated inattention and / or hyperactivity symptoms. Additionally, 43.5% displayed elevated levels of autistic symptomatology and four children (17.4%) displayed severe symptoms at a level which is strongly associated with a clinical ASD diagnosis. In total, 30.4% demonstrated clinically elevated symptoms of both ADHD and ASD. The percentage of children falling within the clinically significant range for ADHD and ASD symptoms in this study was comparable to the proportions found in previous research on NF1 [5,7,19,20,24]. Again, however, it is important to note that there is overlap between the social and cognitive impairments seen in NF1 and ASD, and so the true prevalence of ASD in NF1 may be lower than the literature would indicate [25].
As predicted (Hypothesis 3), children with NF1 and no comorbid ADHD or ASD diagnosis were rated by their parents as having significant social competence problems; group differences in social competence ratings between NF1 children and TD controls remained significant even after excluding NF1 participants with a comorbid psychological diagnosis. However, our hypothesis that social competence would be significantly related to ADHD and ASD symptomatology (Hypothesis 4) was only partially supported. Contrary to predictions, social competence was not significantly related to parent-rated levels of inattention or hyperactivity in our NF1 cohort, nor was social competence related to behavioural indices commonly associated with ADHD, such as defiance / aggression and learning problems. These findings contradict those of previous studies [9,10], which identified children with NF1 and comorbid ADHD and / or learning problems as those most at risk for social problems. Additionally, ADHD is strongly associated with social incompetence in children without NF1 [53,54]. Our results are somewhat surprising and may represent a cohort effect in our relatively small sample. Further study in a larger sample of children with NF1 is certainly warranted to confirm our present findings.
In keeping with expectations (Hypothesis 4), social competence was significantly associated with overall levels of ASD symptomatology in children with NF1, such that individuals with higher ASD symptom levels displayed lower overall social competence. There were significant correlations between social competence and scores on the SRS Autistic Mannerisms treatment subscale (e.g. “has repetitive odd behaviours such as hand flapping or rocking,” “has a restricted or unusually narrow range of interests”) and Social Communication treatment subscale (e.g. “avoids eye contact or has unusual eye contact”, “gets teased a lot”) in the expected direction. It is also interesting to note that a large proportion of the NF1 group (43.5%) demonstrated significant difficulties with social motivation, which taps into socially anxious and avoidant behaviours (e.g. “is too tense in social settings”, “avoids starting social interactions with peers or adults”). This suggests a vulnerability to symptoms of social anxiety in children with NF1 and supports previous research showing a potential predisposition for anxiety disorders in this population [18]. Social Motivation ratings were found to be significantly related to social competence, such that children experiencing increased anxious or avoidant behaviours also displayed lower social competence. Further exploration of social anxiety and its relationship to social functioning in NF1 is warranted, as this may be impacting not only on the ability to form and maintain friendships, but also on emotional and behavioural functioning and overall quality of life in this population. The pattern of results observed in the present study certainly suggests that some combination of autistic traits and social anxiety symptoms might be contributing to the social competence deficits observed in some children with NF1.
The third aim of this study was to explore the relationships between social competence, FSIQ, and executive function in children with NF1. In keeping with expectations (Hypothesis 5), social competence was not significantly related to general levels of intellectual functioning in the NF1 group. However, our hypothesis that lower social competence would be associated with higher levels of day to day executive dysfunction (Hypothesis 6) was not supported. While group means were not significantly different from those reported in published normative data, over half (56.5%) of the children with NF1 in our cohort were rated by their parents as demonstrating difficulty at a clinically significant level in at least one executive domain, supporting previous research showing significant day to day executive dysfunction in this population [12]. Previous studies have shown significant relationships between social deficits and executive dysfunction in typically developing children [42,43], ASD [44,55], and other genetic disorders, including 22q11 deletion syndrome [56], but no existing study has explicitly explored the relationship between social competence and executive function in NF1. While the lack of relationships between functional executive behaviours and social competence are not clear, one possible explanation is that our study solely relied on parent report questionnaires of executive function, which only measure children’s executive abilities in the home environment and so may be less sensitive than other executive function measures. Of note, a previous study investigating the correlations between informant report measures of executive function and neuropsychological test performance in children with NF1 found inconsistent relationships between these variables, suggesting that these measures might tap different constructs [12]. Future research investigating social competence and executive function in children with NF1 should supplement parent reports of executive function with additional measures, including teacher report questionnaires and behavioural assessment tools, such as the Behavioural Assessment of the Dysexecutive Syndrome in Children (BADS-C) [57].
Study limitations
There were several methodological limitations in the present study which must be considered. Firstly, as mentioned above, this study relied solely on parent report questionnaires of social and behavioural functioning. Previous research has demonstrated considerable variations between reports from different informants on social and behavioural rating instruments [58]. Future research investigating social competence in NF1 should corroborate parent ratings with information from additional sources, including teachers, peers, and self-report, to limit the amount of potential bias.
The possibility of response bias must also be considered. Of the 30 sets of questionnaires sent out, only 23 were returned and it is possible that the parents of children with more comorbid symptomatology and / or greater social difficulties were those most likely to choose to participate in the present study. Nevertheless, the descriptive statistics of the 23 responders were in keeping with expectations for children with NF1, and the seven non-responders did not differ significantly from responders with respect to sample demographics.
Finally, it is important to note that the ADHD and ASD symptom questionnaires used in this study were screening tools only. No diagnostic or treatment decisions can be made on these reports alone, as all ratings require confirmation from independent sources. Although 47.8% of our NF1 cohort demonstrated symptoms of ADHD in the “very elevated” range, only 21.7% of these children had a confirmed ADHD diagnosis. Future research investigating the relationship between social competence and comorbid ADHD and ASD should aim to incorporate formal information regarding confirmed diagnostic status in a larger sample to explore more rigorously the influence of these variables on day to day social functioning. This may include a diagnostic interview such as the Schedule for Affective Disorders and Schizophrenia for School-Age Children (K-SADS) [59].
Future research
Further research in a larger sample of children with NF1 will be necessary to confirm and extend the present findings. It is clear that children with NF1 demonstrate significant social competence problems, however, the nature of the relationships between these problems and comorbid ADHD and / or ASD diagnoses warrants further exploration. Studies with larger sample sizes could focus on subgroup analyses based on psychological comorbidities (e.g. NF1 + ADHD, NF1 + ASD, NF1 + ADHD + ASD and NF1 only) to investigate any associated differences in social competence. As stated previously, the inclusion of diagnostic assessment tools for ADHD and ASD would be informative, as would formal screening for social anxiety symptoms. Notably, when exploring the effect of ASD on social competence, it would also be important to understand the possible mediating effect of social anxiety. This could be investigated with formal statistical analyses in a larger NF1 cohort.
There are many other variables which may be important in contributing to social competence problems in children with NF1 which were not explored in the current study. For example, children with NF1 suffer from low academic achievement [17], cosmetic disfiguration [60] and significant impairment in multiple cognitive domains, including attention and language skills [5]. These variables have all been separately associated with social dysfunction in children with mild cognitive and behavioural disabilities [61] and certainly warrant further investigation in children with NF1. Previous research has also identified deficits in social information processing and higher-level social cognition in those with NF1 [34,36] which are likely to contribute to reduced social functioning. Elucidating the potential cause(s) of the social difficulties is an important task for future research, as this information will inform more individualised clinical management and intervention recommendations for children with NF1.
Clinical implications
The present findings indicate a significant risk of social competence problems for children with NF1, even in the absence of comorbid ADHD, reduced intellectual abilities or functional executive difficulties. As such, these findings highlight the importance of screening for social competence problems as part of standard clinical assessment and management protocols for children with NF1. Given questionnaires such as the Social Competence with Peers Questionnaire (SCPQ) [1] are freely available tools with sound psychometric properties that can be completed in less than five minutes, incorporating them into the clinical assessment of children with NF1 is highly feasible. The questionnaire is available in parent (SCPQ-P), teacher (SCPQ-T) and pupil (SCPQ-PU) versions which all correlate strongly in neurotypical children [1].
In keeping with previous research [5,7,20,23,24], we identified elevated levels of ADHD and / or ASD symptoms in a large proportion of our NF1 cohort (including high levels of socially anxious behaviour). Higher levels of ASD symptomatology and socially anxious behaviour were significantly associated with poorer social competence in children with NF1. These findings strongly suggest the need for general psychological screening in children with NF1, particularly those with reduced social competence. While ADHD screening measures such as the Conners 3 rating scales [49] are routinely completed as part of the clinical management of children with NF1 at CHW, the present findings suggest that children with reduced social competence should also be screened for social anxiety and elevated ASD symptoms. The Social Responsiveness Scale (SRS) [22] may be useful as a screening measure for ASD in children with NF1 with poor social competence, providing information about specific problematic behaviours and social skills deficits that will assist clinicians in designing and implementing appropriate interventions. Notably, the SRS also includes a Social Motivation treatment subscale that assesses socially anxious and avoidant behaviours [22]. The Spence Children’s Anxiety Scale (SCAS) [62] could also be administered to children with NF1 and social competence problems as a more general screen for anxiety symptoms.
Children with NF1 who display social competence problems are likely to require interventions targeted at forming and maintaining friendships with their peers. No published studies to date have explored the effectiveness of social intervention programs for children with NF1; however our present findings suggest that it may be suitable to trial treatment interventions designed for children with ASD in an NF1 cohort. In particular, intervention with a focus on social motivation and the management of anxiety surrounding social interactions may be beneficial. Nevertheless, the significant variability observed in the clinical, neuropsychological and social phenotypes of children with NF1 indicates that their social competence problems could reflect a number of individual contributing factors and individualised intervention programs targeting particular skill deficits or problem behaviours may be necessary. Spence [63, 64] advocates a multimodal approach to social skills training for children with social competence problems, including: behavioural skills training (e.g. modelling, role playing, feedback, and reinforcement); social perception skills training; instruction in self-regulation techniques; social problem solving; and parent training. The development and implementation of these programs for children with NF1 will be an important task for future research.
Conclusion
The present findings indicate that children with NF1 are at significant risk of day to day social competence problems, especially those who display high levels of autistic symptomatology and socially anxious behaviour. Nevertheless, social competence problems in NF1 occur even in the absence of comorbid ADHD and ASD and do not appear to be related to general levels of intellectual functioning or functional executive abilities. These results suggest a need to incorporate assessment, prevention and intervention for social problems into the general clinical management of children with NF1, even for those children with relatively normal neuropsychological profiles. Identifying the contributing factors of social competence problems in NF1 and designing appropriate intervention programs will be important challenges for future research.
Acknowledgement
The authors gratefully acknowledge Dr Naomi Sweller for her statistical expertise.
Funding
This research received no specific grant from any funding agency.
Competing Interests
The authors declare that they have no competing interests.
1ADHD was diagnosed in this study based on parent and teacher questionnaire ratings, neuropsychological test performance, and clinical presentation as part of a concurrent study [9].
2The Social Problems index on the CBCL contains only two out of 11 items (“gets teased” and “not liked”) which directly pertains to the quality of children’s relationships with their peers. Similarly, the CBCL Social Competence index contains only two items relating to children’s friendships (“number of friends” and “frequency of contact with friends”).
3One TD control participant fell at the upper end of the borderline IQ range, and two TD participants had IQs > 120, however these participants were not outliers from the TD group as a whole in terms of their SCPQ–P ratings. Notably, FSIQ did not correlate significantly with SCPQ–P ratings in the TD control sample (p = 0.369).
4The mean for the NF1 sample was also compared with the normative mean [1] using the One-Sample Wilcoxon Signed Ranks Test. The NF1 group displayed significantly lower social competence ratings than the normative population (p = 0.033).
References
- Spence SH (1995) Social skills training: Enhancing social competence with children and adolescents. Windsor, Berkshire: The NFER-NELSON Publishing Company.
- Yohay KH (2006) The genetic and molecular pathogenesis of NF1 and NF2. SeminPediatrNeurol13: 21-26.
- Williams VC, Lucas J, Babcock MA, Gutmann DH, Korf B, et al. (2009) Neurofibromatosis type 1 revisited. Pediatrics 123: 124-133.
- Szudek J, Birch P, Riccardi VM, Evans DG, Friedman JM, et al. (2000) Associations of clinical features in neurofibromatosis 1 (NF1). Genet Epidemiol 19: 429-439.
- Hyman SL, Shores EA, North KN (2005) The nature and frequency of cognitive deficits in children with neurofibromatosis type 1. Neurology 65: 1037-1044.
- Huijbregts SCJ, De Sonneville LMJ (2011) Does cognitive impairment explain behavioral and social problems of children with neurofibromatosis type 1? Behav Genet 41: 430-436.
- Garg S, Lehtonen A, Huson SM, Emsley R, Trump D, et al. (2013) Autism and other psychiatric comorbidity in neurofibromatosis type 1: Evidence from a population-based study. Dev Med Child Neurol 55: 139-145.
- Johnson NS, Saal HM, Lovell AM, Schorry EK (1999) Social and emotional problems in children with neurofibromatosis type 1: Evidence and proposed interventions. J Pediatr 134: 767-772.
- Barton B, North K (2004) Social skills of children with neurofibromatosis type 1. Dev Med Child Neurol 46: 553-563.
- Noll RB, Reiter PJ, Moore BD, Schorry EK, Lovell AM, et al. (2007) Social, emotional and behavioral functioning of children with NF1. Am J Med Genet A 143A: 2261-2273.
- Lehtonen A, Howie E, Trump D, Huson SM (2013) Behaviour in children with neurofibromatosis type 1: Cognition, executive function, attention, emotion, and social competence. Dev Med Child Neurol 55: 111-125.
- Payne JM, Hyman SL, Shores EA, North KN (2011) Assessment of executive function and attention in children with neurofibromatosis type 1: Relationships between cognitive measures and real-world behavior. Child Neuropsychol 17: 313-329.
- Rowbotham I, Pit-ten CIM, Sonuga-Barke EJS, Huijbregts SCJ (2009) Cognitive control in adolescents with neurofibromatosis type 1. Neuropsychology 23: 50-60.
- Feldmann R, Denecke J, Grenzebach M, Schuierer G, Weglage J, et al. (2003) Neurofibromatosis type 1: Motor and cognitive function and T2-weighted MRI hyper intensities. Neurology 61: 1725-1728.
- Ferner RE, Hughes RA, Weinman J (1996) Intellectual impairment in neurofibromatosis 1. J NeurolSci 138: 125-133.
- Brewer VR, Moore BD, Hiscock M (1997) Learning disability subtypes in children with neurofibromatosis. J Learn Disabil 30: 521-533.
- Hyman SL, Shores EA, North KN (2006) Learning disabilities in children with neurofibromatosis type 1: Subtypes, cognitive profile, and attention-deficit-hyperactivity disorder. Dev Med Child Neurol 48: 973-977.
- Pasini A, Lo-Castro A, Di Carlo L, Pitzianti M, Siracusano M, et al. (2012) Detecting anxiety symptoms in children and youths with neurofibromatosis type 1. Am J Med Genet B 159B: 869-873.
- Hofman KJ, Harris EL, Bryan RN, Denckla MB (1994) Neurofibromatosis type 1: The cognitive phenotype. J Pediatr 124: S1-8.
- Mautner VF, Kluwe L, Thakker SD, Leark RA (2002) Treatment of ADHD in neurofibromatosis type 1. Dev Med Child Neurol 44: 164-170.
- American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders (5th Eds.) Washington, DC: American Psychiatric Association.
- Constantino J (2002) The Social Responsiveness Scale. Los Angeles, CA: Western Psychological Services.
- Adviento B, Corbin IL, Widjaja F, Desachy G, Enrique N, et al. (2014) Autism traits in the RASopathies. Am J Med Genet 51: 10-20.
- Walsh KS, Vélez JI, Kardel PG, Imas DM, Muenke M, et al. (2013) Symptomatology of autism spectrum disorder in a population with neurofibromatosis type 1. Dev Med Child Neurol 55: 131-138.
- Payne JM (2013) Autism spectrum disorder symptomatology in children with neurofibromatosis type 1. Dev Med Child Neurol 55: 100-101.
- Garg S, Green J, Leadbitter K, Emsley R, Lehtonen A, et al. (2013) Neurofibromatosis type 1 and autism spectrum disorder. Pediatrics 132: e1642-e1648.
- Baio J (2012) Prevalence of autism spectrum disorders - Autism and Developmental Disabilities Monitoring Network, 14 sites, United States, 2008. Morbidity and Mortality Weekly Report: Surveillance Summaries 61: 1-19.
- Belzeaux R, Lancon C (2006) Neurofibromatosis type 1: Psychiatric disorders and quality of life impairment. Presse Med. 35: 277-280.
- Kessler RC, Aguilar-Gaxiola S, Alonso J, Chatterji S, Lee S, et al. (2009) The global burden of mental disorders: An update from the WHO World Mental Health (WMH) surveys. EpidemiolPsichiatrSoc 18: 23-33.
- Bowen R, Chavira DA, Bailey K, Stein MT, Stein MB, et al. (2008) Nature of anxiety comorbid with attention deficit hyperactivity disorder in children from a pediatric primary care setting. Psychiatry Res 157: 201-209.
- Schatz DB, Rostain AL (2006) ADHD with comorbid anxiety: A review of the current literature. J AttenDisord 10: 141-149.
- Bellini S (2004) Social skills deficits and anxiety in high-functioning adolescents with autism spectrum disorders. Focus Autism Other DevDisabl 19: 78-86.
- Bellini S (2006) The development of social anxiety in adolescents with autism spectrum disorders. Focus Autism Other DevDisabl 21: 138-145.
- Huijbregts S, Jahja R, De Sonneville L, De Breij S, Swaab BH, et al. (2010) Social information processing in children and adolescents with neurofibromatosis type 1. Dev Med Child Neurol 52: 620-625.
- Pride NA, Crawford H, Payne JM, North K (2013) Social functioning in adults with neurofibromatosis type 1. Res DevDisabil34: 3393-3399.
- Pride NA, Korgaonkar MS, Barton B, Payne JM, Vucic S, et al. (2014) The genetic and neuroanatomical basis of social dysfunction: Lessons from neurofibromatosis type 1. Hum Brain Mapp35: 2372-2382.
- Descheemaeker MJ, Ghesquière P, Symons H, Fryns JP, Legius E, et al. (2005) Behavioural, academic and neuropsychological profile of normally gifted Neurofibromatosis type 1 children. J Intellectual Disabil Res 49: 33-46.
- Dilts CV, Carey JC, Kircher JC, Hoffman R, Creel D, et al. (1996) Children and adolescents with neurofibromatosis 1: A behavioral phenotype. J DevBehavPediatr 17: 229-239.
- Benjamin CM, Colley A, Donnai D, Kingston H, Harris R, et al. (1993) Neurofibromatosis type 1 (NF1): Knowledge, experience, and reproductive decisions of affected patients and families. Am J Med Genet 30: 567-574.
- Gresham FM, Elliott SN (1990) Social Skills Rating System. Circle Pines, MN: American Guidance Service.
- Achenbach TM (1991) Manual for the Child Behavioral Checklist / 4-8 and 1991 profile. Burlington, VT: University of Vermont, Department of Psychology.
- Razza RA (2009) Associations among false-belief understanding, executive function, and social competence: A longitudinal analysis. J ApplDevPsychol 30: 332-343.
- Riggs NR, Jahromi LB, Razza RP, Dillworth-Bart JE, Mueller U, et al. (2006) Executive function and the promotion of social-emotional competence. J ApplDevPsychol 27: 300-309.
- McEvoy RE, Rogers SJ, Pennington BF (1993) Executive function and social communication deficits in young autistic children. Journal of Child Psychology and Psychiatry 34: 563-578.
- Levine TM, Materek A, Abel J, O’Donnell M, Cutting LE, et al. (2006) Cognitive profile of neurofibromatosis type 1. SeminPediatrNeurol 13: 8-20.
- National Institutes of Health Consensus Development Conference (1988) Neurofibromatosis conference statement. Arch Neurol 45: 575-578.
- Wechsler D (2003) The Wechsler Intelligence Scale for Children - Fourth Edition (WISC-IV). San Antonio, TX: Pearson PsychCorp.
- Wechsler D (1999) The Wechsler Abbreviated Scale of Intelligence Scale (WASI). San Antonio, TX: Pearson PsychCorp.
- Conners CK (2008) Conners (3rd Eds.) Toronto, Ontario: Multi-Health Systems.
- Gioia G, Isquith P, Guy S, Kenworthy L (2000) Behavior Rating Inventory of Executive Function - Professional Manual. Odessa, FL: Psychological Assessment Resources.
- Gioia G, Isquith P, Retzlaff PD, Espy KA (2002) Confirmatory factor analysis of the Behavior Rating Inventory of Executive Function (BRIEF) in a clinical sample. Child Neuropsychol 8: 249-257.
- Rothman KJ (1990) No adjustments are needed for multiple comparisons. Epidemiology 1: 43-46.
- De Boo GM, Prins PJM (2007) Social incompetence in children with ADHD: Possible moderators and mediators in social-skills training. ClinPsychol Rev 27: 78-97.
- Ronk MJ, Hung AM, Landau S (2011) Assessment of social competence of boys with attention-deficit/hyperactivity disorder: Problematic peer entry, host responses, and evaluations. J Abnorm Child Psychol 39: 829-840.
- Ozonoff S, Pennington BF, Rogers SJ (1991) Executive function deficits in high-functioning autistic individuals: Relationship to theory of mind. J Child Psychol Psychiatry 32: 1081-1105.
- Kiley-Brabeck K, Sobin C (2006) Social skills and executive function deficits in children with the 22q11 deletion syndrome. ApplNeuropsychol 13: 258-268.
- Emslie H, Wilson FC, Burden V, Nimmo-Smith I, Wilson BA, et al. (2003) Behavioural Assessment of the Dysexecutive Syndrome in Children. Titchfield, Hants, England: Thames Valley Test.
- Achenbach TM, McConaughy SH, Howell CT (1987) Child / adolescent behavioral and emotional problems: Implications of cross-informant correlations for situational specificity. Psychol Bull 101: 213-232.
- Kaufman J, Birmaher B, Brent D, Rao U, Flynn C, et al. (2008) Schedule for Affective Disorders and Schizophrenia for School Age Children: Present and Lifetime Version (K-SADS-PL). In Rush AJ(Jr), First MB, Blacker D, editors. Handbook of psychiatric measures. (2ndeds). Washington, DC: American Psychiatric Publishing Incpp: 273-378.
- Rosario S (2007) Growing up and living with neurofibromatosis 1 (NF1): A British Bangladeshi case study. J Genet Couns 16: 551-559.
- Gresham FM, MacMillan DL (1997) Social competence and affective characteristics of students with mild disabilities. Rev Educ Res 67: 377-415.
- Spence SH (1997) The structure of anxiety symptoms amongst children: A confirmatory factor analytic study. J Abnorm Child Psychol 106: 280-297.
- Spence SH (2003) Social skills training with children and young people: Theory, evidence and practice. Child AdolescMent Health 8: 84-96.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences